The new standard in eHealth
Enterprise level Occupational Health tools & services that any practice or organisation can afford.
Get in TouchTrusted by companies across Africa




We are relocating!Effective 2 September 2024 to the Agri-Expo Building, Ground Floor Unit 11A, 11 Queen Street, Durbanville.
Enterprise level Occupational Health tools & services that any practice or organisation can afford.
Get in Touch



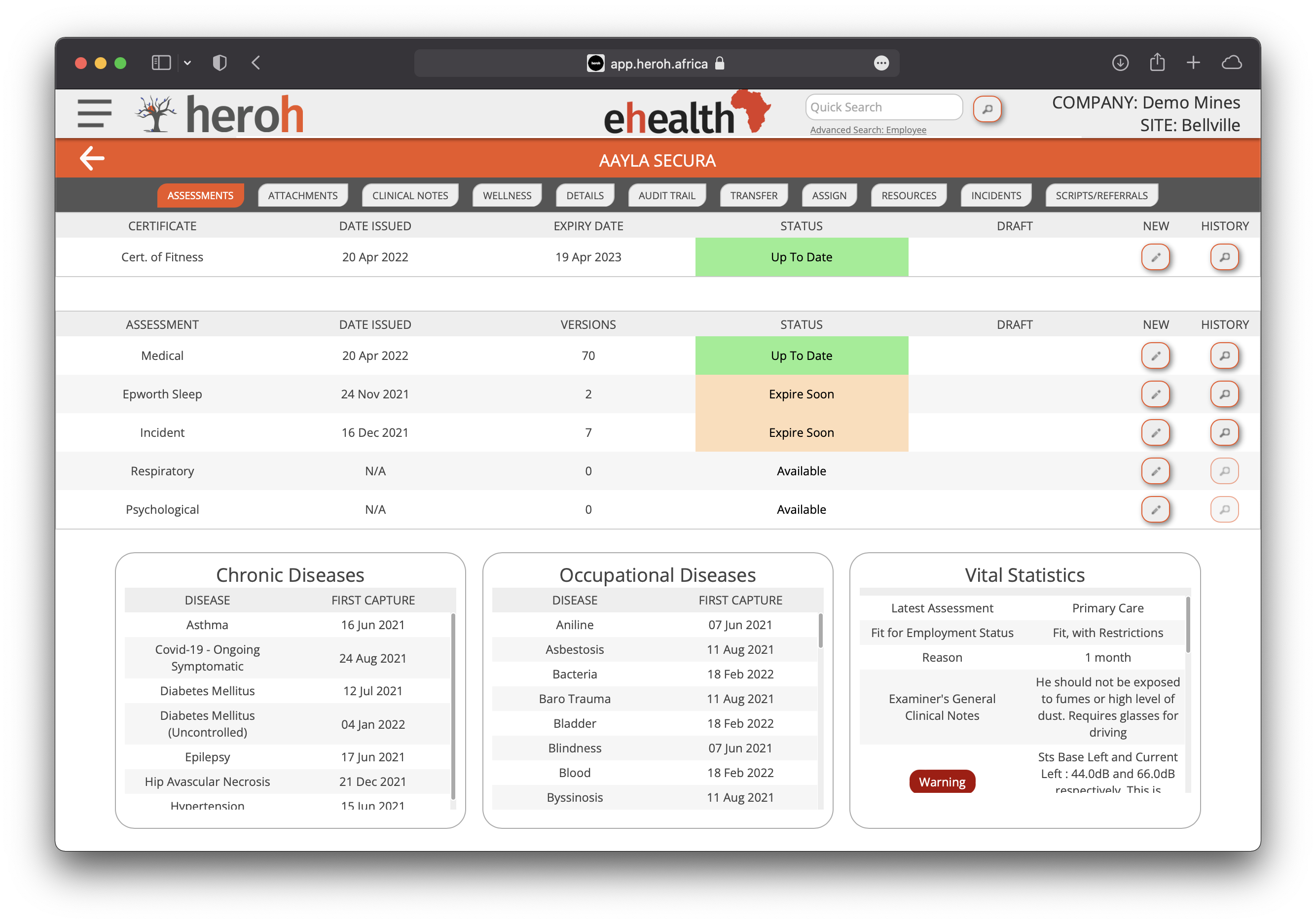
Heroh is a collection of tools used by occupational health practices and their clients to manage and track employee health by issue of a Certificate of Fitness, the industry standard document that certifies an individual as being fit to engage in a particular work activity or industrial project.
Each independent Occupational Health Service Provider (OHSP) signing up to Heroh becomes part of our eHealth Africa network. This network facilitates single source procurement, in other words, by booking with eHealth Africa, companies with an (inter-) national footprint obtain access to standardised, quality assured medical surveillance with risk-based outcomes for its entire workforce, anywhere in (South-) Africa. Make a booking, tell us where and we take care of the rest.

In order to remain current with best practice and to facilitate an incubator for our software, eHealth Africa delivers a direct service from or at our offices in Bellville, to a select group of companies in the Western Cape. This does not imply competing with our Heroh network of OHSP's. Instead, it ensures a quality assured product, cognisant and staying abreast of the industry.
There are many countries where Occupational health is either poorly regulated or not regulated at all. Poor or no regulation implies limited Occupational Health services. Limited Occupational Health services implies a captive market, or even worse, the promotion of unethical behaviour by employers. How to address this quickly? Heroh provides you as a general practitioner in such territories with the tools and Occupational Health framework to make a difference.
Your requirement for bespoke healthcare software development may imply:
Once off delivery of a software solution to resolve and meet a specific operational objective.
Ongoing development of a bespoke healthcare software product, inclusive of maintenance and support.
eHealth Africa will consider any request for bespoke development under option (1). Option (2) may also be considered but in order to avoid concerns regarding conflict of interest, such requests will likely be referred to Smart Africa. Smart Africa is a sister company of eHealth Africa, dedicated to software development services since May 2010.
Initially, we focussed all our energy on Occupational Health: Providing a toolset for Occupational Health practitioners - not only a practice management solution, but a suite of tools to address your needs. And your clients' needs. So we originally set out to provide an enterprise level Occupational Health suite of tools that any practice or organisation can afford. But as we went along, we learnt so much more.
As a result of eating our own lunch (we actively using Heroh ourselves) we've been at the leading edge in medical surveillance services since 2015. Having made lots of mistakes along the road and having learnt so much as we went along, we've gained excellent judgement with regards to best practices.
If you're an Occupational Health Service Provider interested in or already using Heroh, but in need of process optimisation, apart from training your staff we will gladly walk the extra mile.
If you're a company that must implement or adjust a medical surveillance plan, do a health risk assessment or even set up an on site clinic, please contact us. We've done this many times over.
Occupational Health used to be a cost centre. Employers world-wide since realised that Occupational Health provides a framework to protect its most valuable assets - its employees. They realised that Occupational Health safeguards their existence. The increased adoption by employers is why it is crucial that Occupational Health service providers must be equipped with appropriate tools to perform their duty.
Whether existing or new, Occupational Health regulations evolve. For this to happen, data is required. Collective data guides Occupational Health bodies, whether government departments, institutes, service providers, or even employers, to zoom in on areas of concern and facilitate response. But data captured on paper and collecting dust is of very little use.
We focus our entire operation - from our eat-your-own-lunch clinic in Cape Town, to our remote software teams - around 3 core concepts: